
Mental health is an integral part of our overall wellbeing. It affects virtually every aspect of our lives – from our emotional state to daily activities and socialising with others. Different factors affect our mental health: individual biological characteristics, positive and negative lived experiences, relationships with family and social circles.
People from multicultural backgrounds face unique challenges that increase their risk of developing mental illness. Traumatic experiences, displacement, and social integration difficulties deteriorate a person’s psychological wellbeing. And more than that, very often, people from diverse communities are unable to access timely psychological help.
In this article, we’ll discuss:
- What is mental health?
- What factors increase the risks of mental illness in multicultural communities?
- What are the barriers to seeking and accessing mental health support?
- How can mental health services better reach multicultural communities?
Before we start, it’s important to clarify the two terms, which are sometimes confused or wrongly used interchangeably: mental health and mental illness.
Mental health vs mental illness. Definition.
The term mental health refers to our overall psychological wellbeing: our emotions, thoughts and feelings, outlook, problem solving and socialising.
“Mental health is a state of well-being in which an individual realizes his or her own abilities, can cope with the normal stresses of life, can work productively and is able to make a contribution to his or her community. Mental health is fundamental to our collective and individual ability as humans to think, emote, interact with each other, earn a living and enjoy life.”
– World Health Organization
Mental illness refers to various mental health disorders and conditions. These have specific symptoms and negatively affect a person’s wellbeing, thinking and behaviour. The conditions include depression, anxiety disorders, eating disorders, addictive behaviours, and schizophrenia.

Challenges and barriers to accessing mental health support in CALD communities
Mental health in multicultural communities is a systemic issue. On the one hand, migrants, refugees and asylum seekers experience mental illness and suicidal behaviour at significantly higher rates than the general population [1]. Therefore, they should be in a higher need of mental health support, while, in reality, they underutilise healthcare and support services [2]. What are some of the factors that impact people’s mental wellbeing and stop them from seeking prevention and treatment?
Cultural stigma of mental illness
Multicultural communities are more vulnerable due to high mental health-related stigma in their communities.
Firstly, certain cultural and religious customs may prevent people from talking about mental health and using help services. In some societies, mental health is never discussed, and people grow up unaware of the issue [3]. The state of mental distress and suffering may even be normalised [4].
Secondly, many multicultural communities have conservative attitudes to health-related issues. In some cultures, health problems are supposed to be kept private. Family honour is a crucial cultural aspect in many close-knit ethnic communities. So, having an ill member can put a family to shame. That is why people who are feeling unwell do not seek help from professionals and even from family.
Either way, people from some multicultural communities may be reluctant to seek treatment, care and support due to stigma, which makes early identification, prevention and treatment of mental disorders practically impossible [5].
Different healthcare systems
The differences between the healthcare systems in the person’s country of origin and Australia plays a significant role. Mental illness is not treated the same way everywhere. For example, mental health services in some countries only extend to custodial or hospital treatment for very ill or psychotic patients [6]. So, newly arrived migrants may not be aware of the local healthcare system, whether they can access help services and when they should do so.
The impact of discrimination
Minorities, such as newly arrived migrants, refugees and emerging communities, are most susceptible to racism and ethnic discrimination for numerous reasons. Unconscious biases, insufficient cultural awareness and negative portrayals of certain ethnic groups in the media heavily influence people’s attitudes to the “foreigner”.
Lack of social inclusion and continuous exposure to racism inevitably harm migrants’ wellbeing. Intolerance, judgement and communication barriers lead to chronic psychological distress, increasing the risk of mental illness.
The 2014 Victorian Population Health Survey found that Victorian adults who frequently experience racism are almost five times more likely to have poor mental health than those who do not experience racism (Figure 21.3) [7].
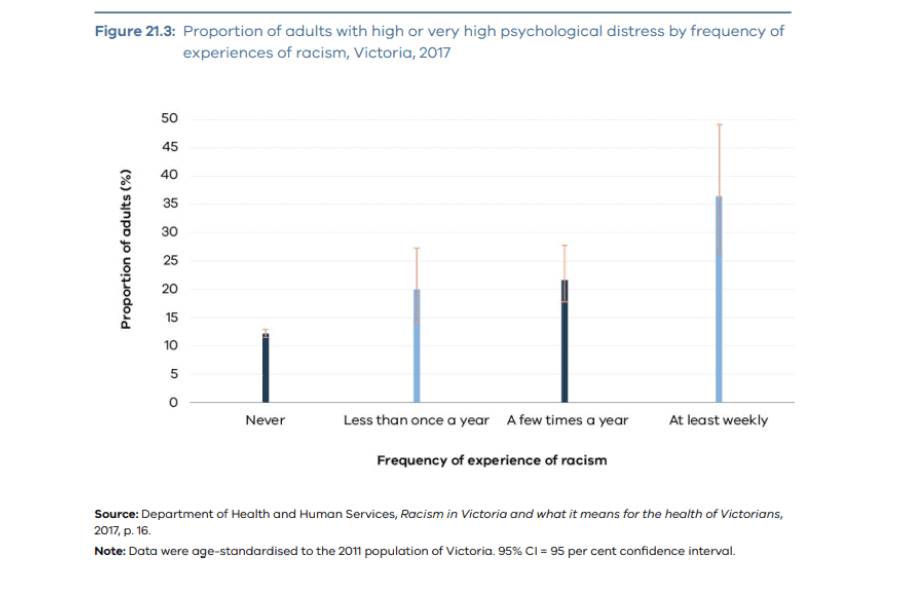
Source: RCVMHS Final Report, Vol.3.
Individuals who experience racism are less likely to seek and access mental health support services. That is because they might expect prejudice or a lack of cultural understanding from the practitioner. The reality is, some practitioners may have a discriminative attitude towards a “foreigner”, even if it is unintentional.
Language barriers
Migrants do not always have sufficient English proficiency to converse comfortably with specialists and express their concerns. Obviously, health professionals are not expected to speak their native language. In-language services or community interpreters are not commonly available. A combination of these factors stops migrants from accessing healthcare services even when it is needed.
“Help” can be traumatising
Naturally, medical facilities need to collect background information from the patient during intake. Then the patient is forwarded to the appropriate specialist, where they have to tell their story over again. For refugees, in particular, this experience is undesired, as they are put to recall and relive the traumatic events, so they may prefer to avoid seeing a psychologist.
Lack of cultural sensitivity and inclusiveness of service providers
Culture shapes how we see the world, react to events, build relationships, and think of the past and the future. To correctly interpret one’s mental condition and provide adequate psychological help, it is crucial to understand the person’s culture. But most often, health specialists are unfamiliar with other cultural belief systems. Often, CALD patients describe mental health services in Australia as being almost exclusively ‘Western’ [8] . This results in the patient and the doctor having two different narratives, misunderstanding and barriers to adequate service provision.
Research is the key to reaching people
Some great organisations provide services to people facing mental health difficulties in Australia. Still, awareness among culturally and linguistically diverse communities is often limited, or if they are aware, they are worried they will face less favourable outcomes than non-CALD individuals. At The LOTE Agency, we provide professional research services and have worked with major mental health providers in Australia to optimise their reach and services. The most rewarding was community engagement and research projects, where we helped organisations identify the communities that need to be reached and understand their unique experiences, requirements, and socio-cultural barriers they face. Our clients find this a huge learning experience, where they recognise that their CALD audiences have specific needs that differ from what they are used to working with.
We explored the issues with ReachOut, headspace and the CMY – watch now
We recently spoke with friends from ReachOut, headspace and the Centre for Multicultural Youth to find out more about mental health in CALD communities, particularly among young people, and the importance of cross-cultural research in mental health communications.
References
1 Mental Health in Multicultural Australia, Introductory Guide: Framework for Mental Health in Multicultural Australia towards Culturally Inclusive Service Delivery, 2014, p. 7
2 Orygen, International Students and Their Mental Health and Physical Safety, 2020, p.6.
3 Evidence of George Yengi, 18 July 2019, p. 1250.
4 Foundation House, Submission to the RCVMHS: SUB.1000.0001.0868, p. 43
5 RCVMHS, Culturally and Linguistically Diverse People Roundtable: Record of Proceedings, 2019
6 Foundation House, Submission to the RCVMHS: SUB.1000.0001.0868, p.12
7 Department of Health and Human Services, Racism in Victoria and what it means for the health of Victorians, 2017, p. 16.
8 Victorian Refugee Health Network, pp. 7–8; Foundation House, Submission to the RCVMHS: SUB.1000.0001.0868, p. 50; Deaf Victoria, p. 9; Ethnic Communities’ Council of Victoria, p. 9.
